May Thurner Syndrome
Vein Specialists of the Carolinas
“All We Do Is Veins, All Day Every Day.”
What Is May-Thurner Syndrome?
May-Thurner syndrome is basically vein symptoms from a blockage of the left leg vein as it goes through the pelvis. The LEFT leg VEIN gets squeezed between the RIGHT leg ARTERY and the spinal column. It can be very hard to tell what causes edema even with lots of medical testing.
Symptoms Include:
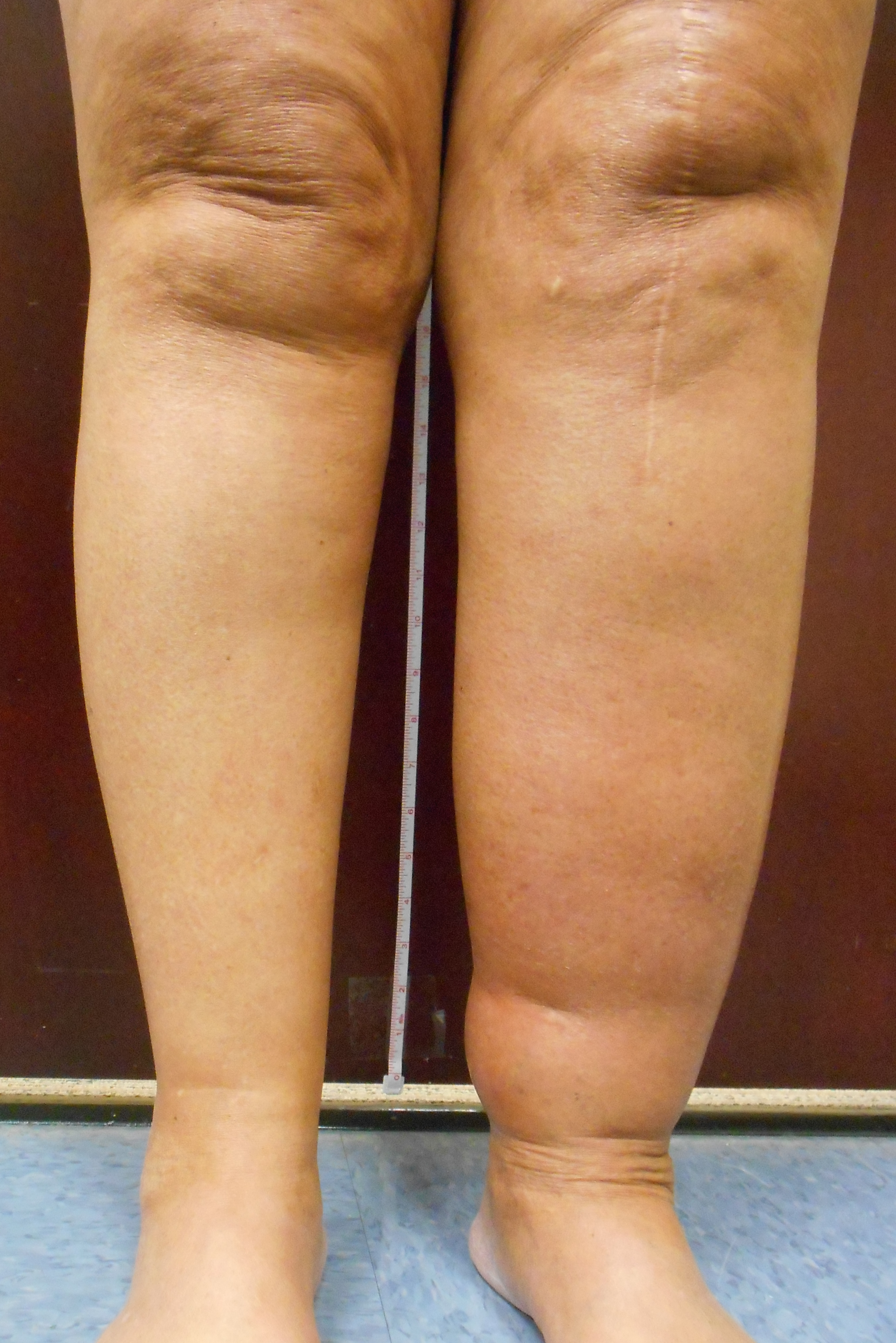
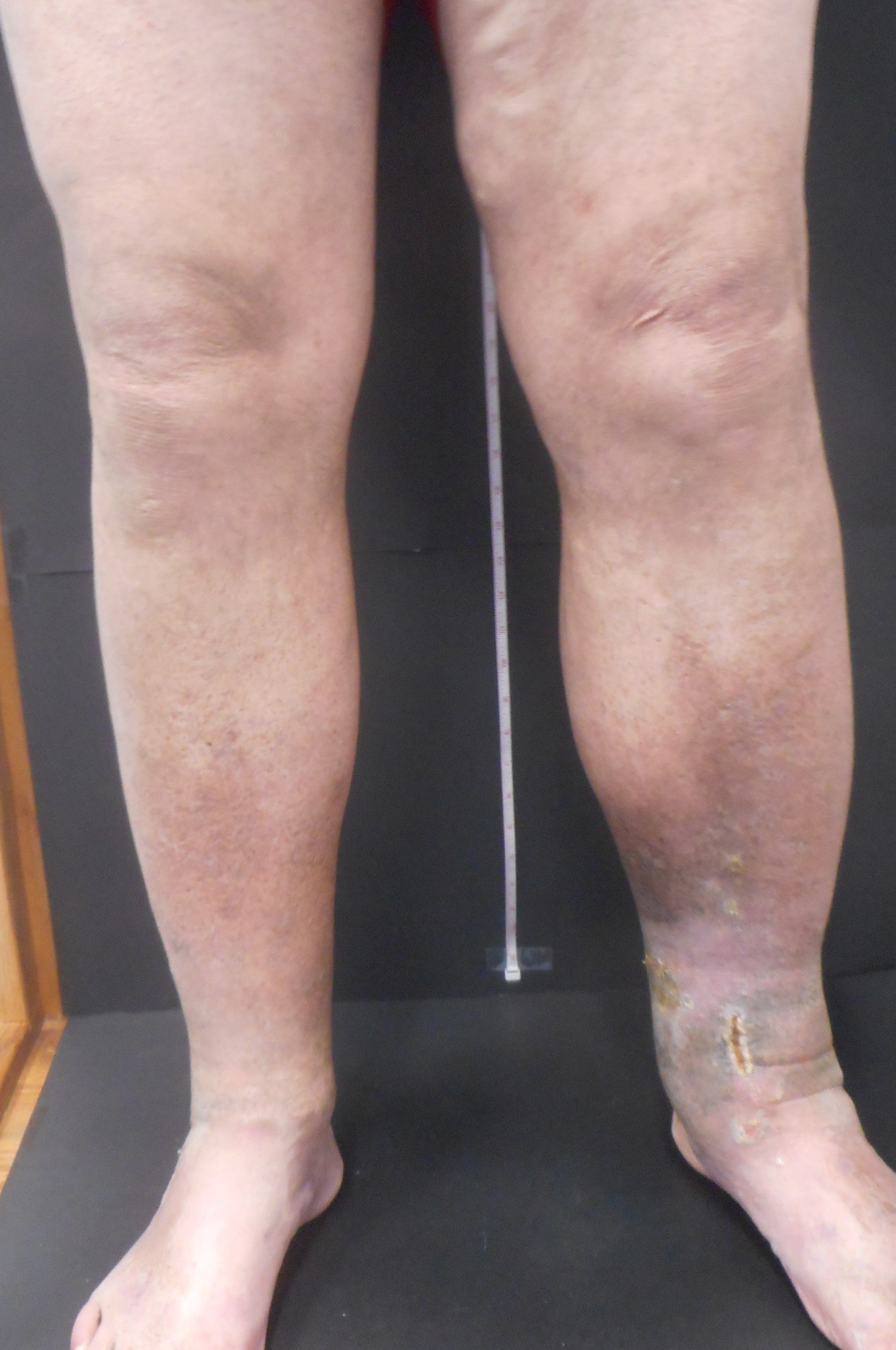
- Pain, heaviness, aching, restlessness, throbbing, varicose veins, leg swelling, leg discoloration or inflammation and leg ulcers.
- Pelvic, hip and back pain can be present
- Varicose veins in areas like the very upper inner thigh, on or underneath the buttock, in the groin area or lower body may be present
- Suspected when vein problems occur early in life—teenage or early twenties. Classic example is tall thin teenage girl with swollen left leg
- It is one reason DVT is more common on the left
- Often found in those with lean body shape
May-Thurner Was Thought To Be Rare
- Today, with better technology, we realize it was just rarely diagnosed
- We also have found it can occur on the right side
- There are 3 areas on each side that commonly get compressed
Since the veins from the pelvic organs, uterus, ovaries, bladder, rectum and gluteal muscles all drain into the leg veins, this blockage can affect them as well.
In women this can lead to pelvic congestion syndrome (PCS) – pelvic pain, urgency to urinate, fullness in the rectum, hemorrhoids, and buttock pain, and possibly pain or aching after sex.
Diagnosing May-Thurner Syndrome
A much more thorough investigation of the veins needs to be done –
once medical causes have been excluded.
Undiagnosed vein problems are a very common cause of swelling.
Ultrasound of the Abdomen and Pelvis with special attention to the veins:
- This test is very difficult to perform accurately. It requires special additional training
- An abdominal and pelvic ultrasound performed by anyone other than a vein specialist will not provide information about the veins.
- This is the newest state of the art technology to diagnose May-Thurner.
- A tiny ultrasound probe on the tip of a long catheter is inserted into the veins where very precise images and videos of the veins can be obtained
- If a blockage of more than 50% is found, Venoplasty and Stenting is the recommended treatment.
At Vein Specialists of the Carolinas we have the cutting edge technology to diagnose and treat this problem in our accredited office based surgical suite.
Dr. Draughn Has Studied With The World's Pioneers and Leading Experts Learning To Diagnose and Treat May-Thurner Syndrome
From The Blog
Understanding May-Thurner Syndrome and Its Impact on Your Veins
May-Thurner Syndrome (MTS), also known as iliocaval compression syndrome, is a vascular condition that affects the veins in the pelvic region, specifically where the left iliac vein passes under the right iliac artery. This anatomical quirk can lead to compression of...
Empowering Women’s Health: Conquering May Thurner Syndrome
In the intricate landscape of women's health, there exists a condition often overlooked and misunderstood: May Thurner Syndrome. This syndrome, also known as pelvic congestion syndrome, manifests as unexplained pelvic pain and discomfort, often misattributed to other...
Understanding Venous Reflux: The Hidden Culprit Behind Vein Problems
Vein problems are often misunderstood and overlooked, but they can significantly impact one's overall health. At Vein Specialists of the Carolinas, we believe that proper understanding of the underlying causes is crucial for effective treatment. One of the primary...
CHARLOTTE, NC
Phone
Hours
Mon.-Thurs.: 7:30am - 4:30pm
Friday: 7:30am-12:30pm
Address
15825 Ballantyne Medical Place,
Ste. 240
Charlotte, North Carolina 28277
GASTONIA, NC
Phone
Hours
Mon.-Thurs.: 7:30am - 4:30pm
Friday: 7:30am-12:30pm
Address
860 Summit Crossing Place,
Ste. 120
Gastonia, North Carolina 28054
From The Blog
Understanding May-Thurner Syndrome and Its Impact on Your Veins
May-Thurner Syndrome (MTS), also known as iliocaval compression syndrome, is a vascular condition that affects the veins in the pelvic region, specifically where the left iliac vein passes under the right iliac artery. This anatomical quirk can lead to compression of...
Empowering Women’s Health: Conquering May Thurner Syndrome
In the intricate landscape of women's health, there exists a condition often overlooked and misunderstood: May Thurner Syndrome. This syndrome, also known as pelvic congestion syndrome, manifests as unexplained pelvic pain and discomfort, often misattributed to other...
Understanding Venous Reflux: The Hidden Culprit Behind Vein Problems
Vein problems are often misunderstood and overlooked, but they can significantly impact one's overall health. At Vein Specialists of the Carolinas, we believe that proper understanding of the underlying causes is crucial for effective treatment. One of the primary...









